EHS is the Leading Preventable Cause of Death Among High School Athletes
Despite Exertional heatstroke (EHS) training and prevention being readily available for high school coaches through California-mandated classes, student-athletes have continued to perish. In an effort to gain a competitive edge, many push their student-athletes beyond their point of physical endurance and student-athletes suffer as a result. Perhaps It’s because although heatstroke is common, it is most often associated with elderly individuals and not with young student-athletes who should have their whole lives in front of them. Unfortunately, this misconception could be the reason EHS isn’t taken seriously enough, however, foundations like the Korey Stringer Institute, an exertional heat stroke prevention institute based out of the University of Connecticut, are working to educate the public and perhaps save some lives.

What Causes the Different Types of Heatstroke?
Different types? Yes. There are two types to contend with. According to the New England Journal of Medicine, “classic heatstroke is due to exposure to environmental heat and poor heat-dissipation mechanisms, whereas exertional heatstroke is associated with physical exercise and results when excessive production of metabolic heat overwhelms physiological heat-loss mechanisms.”
Simply put-an increase in core body temperature brought on by intense physical activity in hot weather causes EHS. Anyone exercising or working in hot weather can get EHS, but it’s most likely to occur if you’re not used to high temperatures.
EHS generally occurs in young individuals who engage in strenuous physical activity for a prolonged period in a hot environment. Classic non-exertional heat stroke (NEHS) most commonly affects sedentary elderly individuals, persons who are chronically ill, and very young persons.
—New England Journal of Medicine
Other factors that affect how EHS can strike someone are:
- Wearing excess padding, sporting equipment, or clothing that prevents sweat from evaporating easily and cooling your body
- Drinking alcohol, which can affect your body’s ability to regulate your temperature
- Becoming dehydrated by not drinking enough water to replenish fluids lost through sweating
How is EHS Diagnosed?
The two main criteria for diagnosing exertional heat stroke (EHS) are rectal temperature >105°F (40.5°C) immediately post-collapse and central nervous system (CNS) dysfunction (e.g. irrational behavior, irritability, emotional instability, altered consciousness, collapse, coma, dizziness, etc.)
The chart below by the New England Journal of Medicine shows what effects EHS has on the body, including cardiac and central nervous system effects.
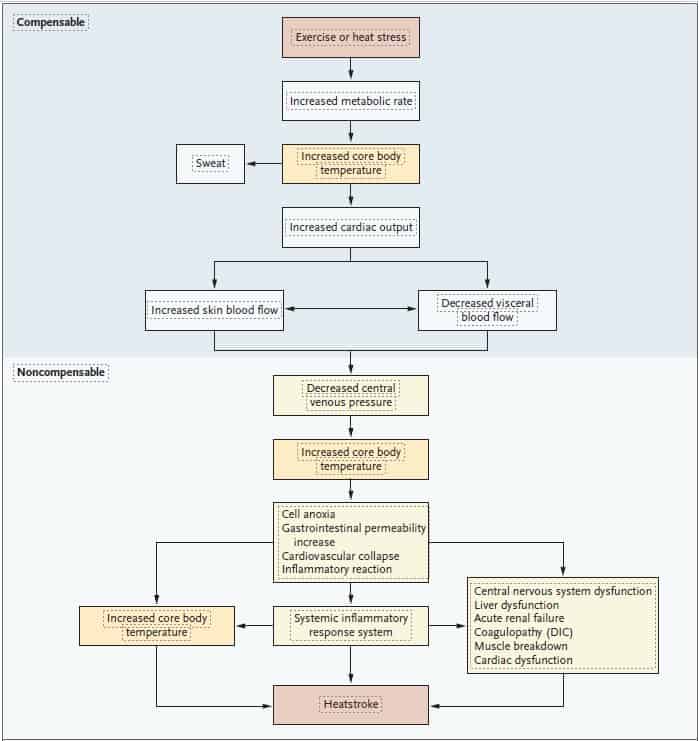
When observing student-athletes, look for these other signs and symptoms that may show they are suffering from EHS:
- Irrational behavior, irritability, emotional instability
- Altered consciousness, coma
- Disorientation or dizziness
- Headache
- Confusion or just look “out of it”
- Nausea or vomiting
- Diarrhea
- Muscle cramps, loss of muscle function/balance, inability to walk
- Collapse, staggering or sluggish feeling
- Profuse sweating
- Decreasing performance or weakness
- Dehydration, dry mouth, thirst
- Rapid pulse, low blood pressure, quick breathing
- Other outside factors may include:
- Weight
- Climate and humidity
- Practice is near the start of the season, and near the end of practice
- It is the first day in full pads and equipment
If a student-athlete collapses during or immediately after exercise, consider EHS as a possible diagnosis. However, collapse is not required to consider EHS. Many student-athletes may display CNS dysfunction without collapse and healthcare professionals should still consider EHS as a possible diagnosis.
Treatment
Heatstroke treatment centers on cooling your body to a normal temperature to prevent or reduce damage to your brain and vital organs. To do this, your doctor may take these steps:
- Immerse you in cold water. A bath of cold or ice water has been proven to be the most effective way of quickly lowering your core body temperature. The quicker you can receive cold water immersion, the less risk of death and organ damage.
- Use evaporation cooling techniques. If cold water immersion is unavailable, health care workers may try to lower your body temperature using an evaporation method. Cool water is misted on your body while warm air is fanned over you, causing the water to evaporate and cool your skin.
- Pack you with ice and cooling blankets. Another method is to wrap you in a special cooling blanket and apply ice packs to your groin, neck, back and armpits to lower your temperature.
- Give you medications to stop your shivering. If treatments to lower your body temperature make you shiver, your doctor may give you a muscle relaxant, such as a benzodiazepine. Shivering increases your body temperature, making treatment less effective.
If you or a loved one has suffered injuries or tragically lost someone because of EHS associated with negligence, visit our wrongful death or catastrophic injury pages to learn more about what your next steps could be. At Adamson Ahdoot LLP, we fight aggressively for those wronged by the harmful actions of others.


































